By Terrah Baker“This is like Christmas,” one attendee of an informational meeting on the Affordable Health Care Act held at Fayetteville Public Library said. “I can’t believe this is real.”This Fayetteville resident had struggled for more than six years to find affordable health insurance due to a pre-existing condition and being laid off from her job. She settled on a plan that cost more than $300 a month, so was ecstatic when the ACA became the law of the land. This meant she could finally get comprehensive coverage at a reasonable cost.
By Terrah Baker“This is like Christmas,” one attendee of an informational meeting on the Affordable Health Care Act held at Fayetteville Public Library said. “I can’t believe this is real.”This Fayetteville resident had struggled for more than six years to find affordable health insurance due to a pre-existing condition and being laid off from her job. She settled on a plan that cost more than $300 a month, so was ecstatic when the ACA became the law of the land. This meant she could finally get comprehensive coverage at a reasonable cost.
Her story is common and a rallying cry amongst the ACA supporters. Now the ACA is rolling out — along with some unfortunate and not well understood website problems — opinions and reports are contradictory, making it hard for the average American to make sense of it all.
While many, like the Fayetteville resident, say it’s the break they’ve been waiting for, others claim the ACA is forcing their insurance companies to drop their policies, raise rates and is just adding more cost to already stretched middle class Americans.
The questions of whether or not the ACA is causing premiums to rise or fall, and how it’s helping the uninsured and insured alike, are hard to answer when analyzed amongst the confusion of such conflicting messages.
First, it’s important to look at what’s at stake. For individuals, it’s health and livelihood; for politicians, it’s re-election and voter approval; for corporations who already make billion-dollar profits on health insurance, it’s not much.
Medicaid — $0 Premiums
“We’re very excited about the (ACA) because we think it will be very helpful to the clients we serve,” Washington County Health Department’s director, Robin Thomas, said. “We see a large portion of the uninsured already in this county and we think this will really be able to help them get health care. Not only with us, but also with other providers.”
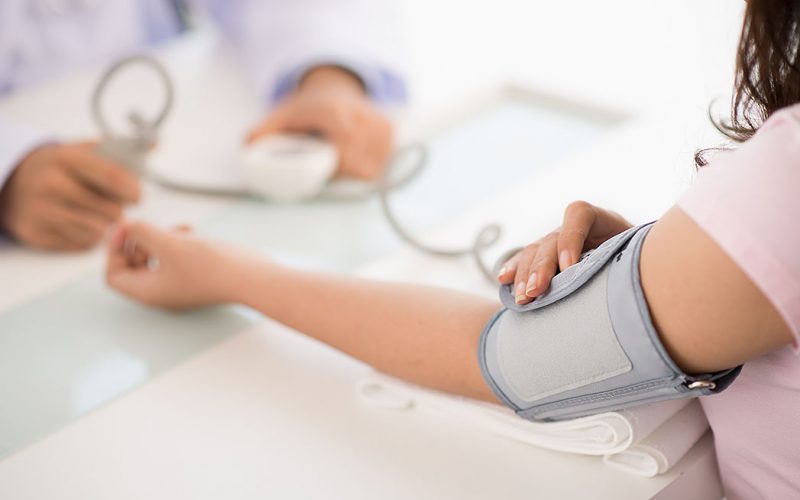
Because Medicaid expansions came along with the ACA, many of the Medicaid recipients that use the Health Department will not only get the services they received before, but also preventative services that were not offered previously. For instance, if a patient on Medicaid had a chronic illness or high blood pressure, and couldn’t afford to go to a physician out of pocket, they had no option but to wait until it became an emergency room visit or serious health issue. Now, they have access to doctors to maintain health, before illnesses get to the dangerous levels. And like before, Medicaid premiums equal $0.
“(Preventative services like family planning, immunizations) are available in our offices now, but the (ACA) will enable them to go see private providers for other visits, for regular check ups. If they’re sick or they have a cold or high blood pressure or some of those things we don’t care for in this clinic, they’ll be able to go to other entities to get those services,” Thomas said.
Brandie Cooper is an In-Person Assister with Arkansas Health Connect and Friendship Community Care — individuals specifically trained on the Health Care Act to help people sign up and find the right options for them. She was hosting the informational session at Fayetteville Public Library, and explained that an individual making up to $15,856 a year is eligible for the $0 premium, as well as two people making up to $21,404, and four people making up to $32,499.
Tax Exemptions
Recently, there’s been many reports of insurance companies dropping people from their health care plans. In their place are plans with higher premiums or a call to enter the marketplace where they’ve been told to expect premiums as high as $300 a month for regular coverage. What the letters aren’t saying is that with those plans they can expect tax exemptions as long as their income is lower than $95,000 a year for a family of four. And that they have three different options for coverage — Gold, Silver and Bronze. Plus, these new marketplace plans have more comprehensive coverage, meeting the new standards set out by the ACA.
People who qualify can expect a monthly premium from $19 and up. For an individual, the tax exemption income cap is set at $45,960 a year, and for a family of two it’s $62,040.
So what if you make more than that? Well, from what insurance companies are saying, your premiums are about to go up.
One political activist and director at MO-Political has said what’s unfortunate about the ACA rollout is that inherently it doesn’t call for the raising of premiums — although requiring companies to offer more comprehensive coverage and take on insurees despite pre-existing conditions might imply that — but insurance companies are taking advantage of the system to make more profit for themselves.
“Insurance companies are using the confusion around the (ACA) to cancel plans altogether and offer replacements with much higher premiums — all without telling people that they have other options and that most people are eligible for tax credits on top of that. Most people who are getting cancellation notices only know that their insurance company discontinued their plan and replaced it with a much more expensive one, while the insurance company blames the ACA in the letter. The truth is that most of these folks are eligible for much better and much more affordable rates through the health care exchanges — but insurance companies don’t want us to know that because they want to make more money for themselves,” Courney Cole of MO-Political said.
One attendee at the FPL verified this, saying employees of the company where she serves as human resources director received letters notifying them that they should enroll in the ACA marketplace and could expect premiums sometimes three times higher than what they were paying.
“The truth is I think their (insurance company) is preparing them to switch over because their own premiums are about to go sky high as of 2014,” she said.
This is something Republicans and opponents of the ACA warned against. And since the idea to have a public cost share option was denied, and few regulations on premium hikes were put in place, it looks like their speculations of rising premiums may be true.
Fears Realized
“In the average state, (ACA) will increase underlying premiums by 41 percent. As we have long expected, the steepest hikes will be imposed on the healthy, the young and the male. And (ACA)’s taxpayer-funded subsidies will primarily benefit those nearing retirement — people who, unlike the young, have had their whole lives to save for their health-care needs,” reported Forbes magazine Nov. 4, citing a study done by the Manhattan Institute — a conservative think-tank.
While the Health Care Act does put protections in place that weren’t there before, and offers low income residents options they didn’t have — including closing the gap between men and women’s insurance and decreasing costs for older Americans — the already hard-hit middle class and young adults are seeing the worst of the fallbacks.
However, reports — and the way insurance works — imply that in early 2014, prices are expected to go down as the costs are spread amongst more people. As a theory, that would mean the premium increases will eventually go down, once the dust and confusion settles.
Conclusion
The conclusion to the statistics show there are no sure conclusions. As of now, premium prices have risen, while prices for low income Americans are wavering on a thin line of affordability, while poverty level Americans are seeing an increase in coverage with little to no premium. Along with that, many say their coverage is better and more comprehensive and deductibles have gone down.
A little more than 14,0o0 Arkansans have applied for health insurance coverage, as reported by the Department of Health and Human Resources (because Arkansas is rolling out the ACA through a partnership with the Federal government, they’re not collecting their own numbers). Of those, 6,123 were eligible for traditional private health insurance plans, with 2,279 qualifying for premium assistance.
Commissioner Jay Bradford expects those numbers to increase as the Dec. 15 deadline nears, and only time will tell if that increase means a decrease in some unfortunate premium hikes.
Getting Insurance
Although the Dec. 15 deadline is for health insurance that will kick in Jan. 1, an extension is in place that will allow people to sign up until Feb. 15 when insurance would kick in March 1. IPAs are specially-trained individuals who are helping people get enrolled and understand their options. They can be found at the Washington County Department of Health and at places like Arkansas Health Connect. To find out more, visit www.healthcare.gov.
How the ACA is funded:
Partly by a tax from individuals making $200,000 and over, couples making $250,000 and over, businesses with a revenue of over $250,000, and the health care industry.